Dental diagnosis In Bellevue, WA
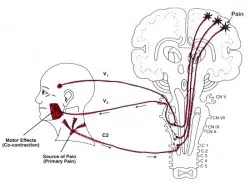
Diagnosis of acute pain is easy and clear because a particular body part has gone the wrong manifest. However, the diagnosis of chronic pain and TMJ disorders are difficult because there is often a disconnection between the source of the pain and the pain experience. It is difficult to assess pain objectively, to adjust to the condition, and often times the best measure of chronic pain intensity is the patient’s word. If you have an incorrect diagnosis and treat it accordingly, your pain and dysfunctions will not go away. Further, you very well may end up traveling from office to office in an attempt to relieve the pain and find out causative factors. The following is a typical example:
I am a 45 year old female. I found your website while I was searching on google for some diagnosis for all my problems. I know I have TMJ as my jaw has been popping and clicking for as long as I can remember. I have been having headaches, neck pain, shoulder pain, arm pain, tingling in my arms and hands, teeth pain, etc. off and on for years. Every couple of years my neck will ‘go out’ and I will go to a chiropractor for a few weeks. I started going to a chiropractor last October for neck pain and headaches. This time I got worse instead of getting better. I started getting severe headaches, severe tingling in my arms and hands and twitching in my right hand. I was referred to an orthopaedic doctor in May (06). I have had several MRI’s (brain, neck and lumbar). I have pinched nerves and bulging discs in my neck. I was referred to a neurologist because my doctor wanted to rule out MS. After testing by the neurologist, it was determined I didn’t have MS and was turned back over to my orthopaedic doctor. He sent me to a pain specialist to get a steroid shot in my neck, hoping it would relieve my headaches enough so I could go through physical therapy for my neck. We waited two weeks after the injection to see if it was going to help with my headaches. I did get some relief. Some days I didn’t have a headache at all (which for me is extremely rare.) I started physical therapy about 3 weeks ago. After the third session, I woke up the following day with the worst headache of my life that lasted for almost two days. I called my doctor and he discontinued physical therapy and decided it is time for me to go to an orthopaedic surgeon for another opinion. I have an appointment to see the surgeon tomorrow. And I have another appointment for another injection in another part of my neck. I told my doctor that I am ready for surgery if it will help ease my pain. I don’t know how much more I can deal with. As I sit here typing this email, I have a fairly severe headache (I woke up with it this morning), my arms are tingling and my shoulders and neck hurt. Please send me any information you can.
Sincerely,
Finding out the true source of pain is critically important and is the key factor for the treatment. Such, multiple diagnostic procedures are developed: medical-dental history, clinical examination, dental examination (intra-oral and extra-oral), occlusion analysis, jaw and neck range of motion, cranial nerve screening, skeletal morphology and posture evaluation, muscle palpation, bio-mechanical functional test, TM joint x-ray and required imaging, electro-diagnostics (jaw joint vibration analysis, jaw tracking analysis), listening to the jaw joint sound, diagnostic splint, orthopedic jaw casts, diagnostic photograph, TMJ scale, diagnostic anesthetic block, etc. However, all these diagnostic procedures do not necessarily provide doctors an accurate diagnostic information or treatment protocol.
Because the majority of chronic pain and TMJ disorder symptoms are pain (location, severity, frequency, duration) and dysfunction (inability for certain body movements), an objective clinical assessment and evaluation of the relationship between pain/dysfunction and TMJ is very important. If the patient responds positively during assessment and evaluation sessions, it enables practitioners to create and implement a treatment protocol with confidence, and except successful treatment outcome.
Dr. Uparika Sharma uniquely developed a simple on-site assessment and diagnostic program, which enables him to identify the true source of pain and dysfunction objectively, whether the symptoms are related with TMJ, and whether the symptoms can be improved with treatment or not.
Treatment
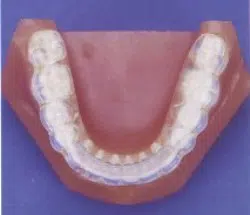
The goal of the treatment is to relieve pain, improve function, and maintain a pain free condition. The primary goal of acute pain treatment is to find the source and provide pain relief. Generally, chronic pain treatment is poor in medical outcomes, the definitive treatment procedure is not clear, and multiple treatment modalities are utilized case by case: various medications, around-the-clock analgesia, time release-opioid, trigger point injection, nerve ganglion block injection, physical therapy, prolotherapy, T.E.N.S., infrared therapy, laser therapy, iontophoresis, stretch and spray, acupuncture, acupressure, neuromuscular massage, biofeedback, craniosacral therapy, chiropractic manipulation, nutritional evaluation, various intraoral orthotic (splint), functional jaw orthopedic appliance, NTI-tss, anterior repositioning appliance, orthodontic teeth and jaw correction, and comprehensive dental work.
There are some recommended “self-care” treatment options: resting the jaw and taking the pressure off from the joint; keeping the teeth apart and refraining it from clenching; keeping the head, neck, and back up-straight to maintain a good jaw posture; eating soft food, applying ice and heat, exercising the jaw in order to restore a normal range of movement; and other relaxation techniques.
Oftentimes, even after attempting all these treatment procedures, you may end up disappointed. Additionally, some estimate as high as 90% of individuals with baseline pain, state that control is unstable, and continue to experience “breakthrough” pain. This warrants reassessment of the cause and approach for management of chronic pain requires stronger or additional pain medications, which may cause various side effects and create new problems, and attempts to utilize non-pharmacologic multidisciplinary modalities. Thus, the goal then becomes management instead of treatment, which would allow the patient to go to work, walk around, clean the house, do outdoor activities, etc.
It is necessary to develop greater sophistication and efficiency in the assessment, diagnosis, definitive treatment, and management of pain and dysfunction. Based on thousands of hours of continuing education, hands-on courses, extended knowledge, and clinical experience in general dentistry, basic medicine, toxicology, neuromuscular dentistry, orthodontics, holistic dentistry, dental sleep medicine, nutritional supplements, allopathic medicine, and oriental medicine, Dr. Uparika Sharma developed a comprehensive but simple assessment and treatment protocol, which he utilizes over 95% of the time with great success and patient satisfaction.